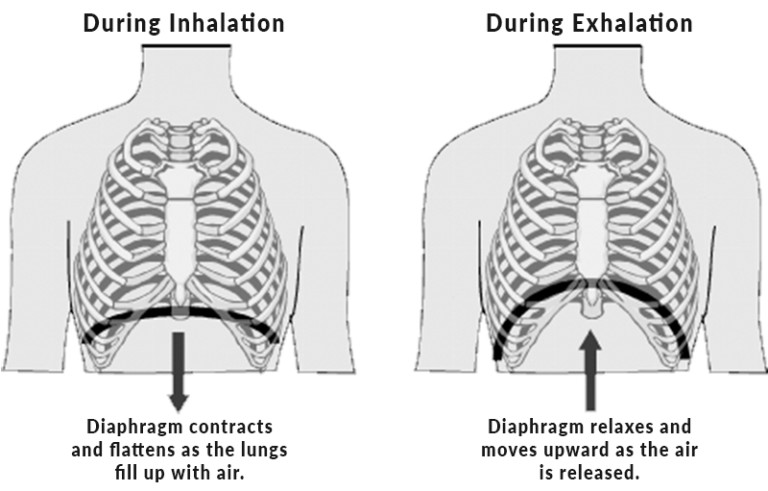
Lead author: Paul Cooley
Lead author: Paul Cooley
Additional contributing author: David Deppeler
Running is a remarkable sport for both its instinctive origin and as a foundation for other physical activities. We all grew up practicing it without any thought, and while many continued training towards running mastery, other’s lost their natural stride and work hard to reestablish this as part of their later lives. There is a refreshing simplicity to running, and it is often a vital component of training for all manners of physical conditioning.
As a distance athlete, you seek to optimize your performance. You realize that even minor dysfunctions can become big roadblocks in training and performance. We have designed unique programs to improve many running variables, but frequent illusive obstacles often persist; side stiches, overwhelming exhaustion under stress, poor recovery post-exercise, recurrent injuries, inefficient running biomechanics and many more common barriers may originate in a silent problem as simple as running itself: breathing.
While you might not realize it, breathing may be one of the most significant barriers to your performance, and one that no one is talking about. Breathing can also play out to be one of your biggest competitive edges. Better breathing does not have to involve working harder at breathing. Quiet contrarily, we hope to show you how to work less and get more from your breath.
This article hopes to help bring breathing back into the discussion and offer some introductory tools to get your breath working for you instead of against you. To completely delve into the realm of breathing dysfunction is well beyond our means here. We simply want to shine a light on an area of training that the running community has historically left unaddressed, introduce some basic self-assessment techniques, and provide insight towards a general treatment pathway to get you heading in the right direction. While we realize many of the techniques here presented may take a bit of self-discovery and practice, many of them are shockingly easy – with fast-occurring results that help inspire practice.
Why is this important?
As respiration is an automatic process under normal circumstances, it is often ignored until a problem arises. When starving for oxygen, suffering a side stich, or experiencing any other symptoms soon to be outlined, it is easy to jump to the assumption that “better breathing” means “more oxygen”. However, this is not the full truth and even during the most strenuous bouts of activity our body fails to use most of the oxygen brought into the lungs. Once it sinks in that “more oxygen” should really be “how do I better use the oxygen that I am already breathing” then the biggest barrier to better breathing is tackled: our own basic breathing patterns and stress response.
This is where we find the crux of common breathing difficulties summarized as Breathing Pattern Dysfunctions. This issue is the topic of our discussion and has been proposed for nearly a century, but only began to gain significant traction amongst healthcare professionals in the last few decades. In regard to sport, Breathing Pattern Dysfunctions can be summarized as an improper response to stress or exercise, in which the breathing rate is changed at a disproportionate rate to tissue demands, and natural muscle recruitment for respiration is inefficient. Breathing Pattern Dysfunctions exist on a spectrum with the far majority being towards the end we summarize as Hyperventilation Syndrome. This term is improperly ascribed towards anxiety attacks and can often exist at rest or without any awareness.

 Athletes commonly encounter respiration performance barriers and are frequently diagnosed with several common dysfunctions, among the most frequent being Exercise Induced Asthma and Vocal Cord Dysfunction. While both diagnoses might sometimes truly exist on their own, other times they might also simply be one symptom within a broader symptom cluster more appropriately classified as a breathing dysfunction. One research group investigated adolescent athletes with diagnosed Exercise Induced Asthma and found that 13% truly showed the classic symptoms of pseudo-asthma, while 34% showed symptoms indicating hyperventilation (Seear, 2005). While most people find some sort of solace in discovering a definitive cause for their ailment, Breathing Pattern Disorders are more like a bad habit, which has been so regularly practiced it has become established as the natural pattern. (Lum, 1975)
Breathing dysfunctions do more than just alter efficient gas exchange and lend to running inefficiency, it also has an influence on muscle tone and can manifest as chronic muscular pain. Low back pain is the most common source of sidelining injury from a wide spectrum of sports and intimately connected with the muscles and mechanics of breathing (Bahr et al, 2004 | Hodges, 2000). The diaphragm coordinates with the abdominals to not only ensure effective breathing but also provide dynamic postural stability to the spine. This is especially important for athletes who ask tremendous efforts from their body. Ultrasound imaging has shown tremendous association between the ineffective firing of the diaphragm/abdominal complex and low back pain (Hodges, 2000). This is an area where simple core exercises may not be the solution and may even be detrimental, as the appropriate synchronous firing of these muscles during respiration and activity cycles takes precedence over outright strengthening.
Training progress hinges on our ability to train hard and recover well, and current research tells us that even minor breathing dysfunctions can compromise our ability to do both. Runners with relatively innocuous breathing inefficiencies can see a decreased capacity for recovery after hard training sessions, increased muscle soreness in the shoulders, back, neck and chest, diminished blood supply to needy muscles, nagging side stitches, constricted collagen in ligaments and fascia, muscle cramps/spasms, and a decreased oxygen transport. During a race, the symptoms often escalate as effort or suspense builds. We have even seen Olympic level athletes display this pattern at the end of a race, when the kick is in full swing and tensions high. It’s not always about “hitting the wall” or “running out of kick”. Sometimes the body is just responding to improper preparation over the first 90% of the race.
Athletes commonly encounter respiration performance barriers and are frequently diagnosed with several common dysfunctions, among the most frequent being Exercise Induced Asthma and Vocal Cord Dysfunction. While both diagnoses might sometimes truly exist on their own, other times they might also simply be one symptom within a broader symptom cluster more appropriately classified as a breathing dysfunction. One research group investigated adolescent athletes with diagnosed Exercise Induced Asthma and found that 13% truly showed the classic symptoms of pseudo-asthma, while 34% showed symptoms indicating hyperventilation (Seear, 2005). While most people find some sort of solace in discovering a definitive cause for their ailment, Breathing Pattern Disorders are more like a bad habit, which has been so regularly practiced it has become established as the natural pattern. (Lum, 1975)
Breathing dysfunctions do more than just alter efficient gas exchange and lend to running inefficiency, it also has an influence on muscle tone and can manifest as chronic muscular pain. Low back pain is the most common source of sidelining injury from a wide spectrum of sports and intimately connected with the muscles and mechanics of breathing (Bahr et al, 2004 | Hodges, 2000). The diaphragm coordinates with the abdominals to not only ensure effective breathing but also provide dynamic postural stability to the spine. This is especially important for athletes who ask tremendous efforts from their body. Ultrasound imaging has shown tremendous association between the ineffective firing of the diaphragm/abdominal complex and low back pain (Hodges, 2000). This is an area where simple core exercises may not be the solution and may even be detrimental, as the appropriate synchronous firing of these muscles during respiration and activity cycles takes precedence over outright strengthening.
Training progress hinges on our ability to train hard and recover well, and current research tells us that even minor breathing dysfunctions can compromise our ability to do both. Runners with relatively innocuous breathing inefficiencies can see a decreased capacity for recovery after hard training sessions, increased muscle soreness in the shoulders, back, neck and chest, diminished blood supply to needy muscles, nagging side stitches, constricted collagen in ligaments and fascia, muscle cramps/spasms, and a decreased oxygen transport. During a race, the symptoms often escalate as effort or suspense builds. We have even seen Olympic level athletes display this pattern at the end of a race, when the kick is in full swing and tensions high. It’s not always about “hitting the wall” or “running out of kick”. Sometimes the body is just responding to improper preparation over the first 90% of the race. What is dysfunctional breathing (and what does it look like)?
Dysfunctional breathing is a habitual tendency to breath at a rate disproportionate with that needed for the activity, and with muscles not designed as primary breathing muscles. As an example, even at very low exercise intensity someone with dysfunctional breathing tends to breath very rapidly and with decreased diaphragm involvement, instead favoring secondary muscles of the chest, shoulders, and neck to pull the lungs open. This pattern poorly fills the lungs at a much higher energy cost, so the athlete tends to take rapid shallow breaths instead of the appropriate slower, deeper breaths. It is becoming well understood that many of these breathing inefficiencies originate through an engrained pattern in an otherwise automatic body process. What might have been a very subtle problem originally can grow more and more pronounced with repetition and training of poor patterning. We don’t have any pump for breathing, instead relying on increasing the volume of our chest to pull air in through a pressure gradient. Ideally, we use mostly the diaphragm to pull down into our abdomen on inhalation, but many muscles attach to the chest and any of these can also get the job done. By constantly practicing an abnormal breathing pattern, it becomes engrained as the automatic pattern the body turns to for respiration.
After struggling for several years with sudden fatigue and shortness of breath at the end of races, the realization that re-learning and practicing proper breathing technique has made a huge difference in my performance. I am able to run better workouts and have seen improvements in my races because I have better body composure and less tightness in my upper back and shoulders.
Jordan Hasay - Professional Runner

What hyperventilation does to your body:
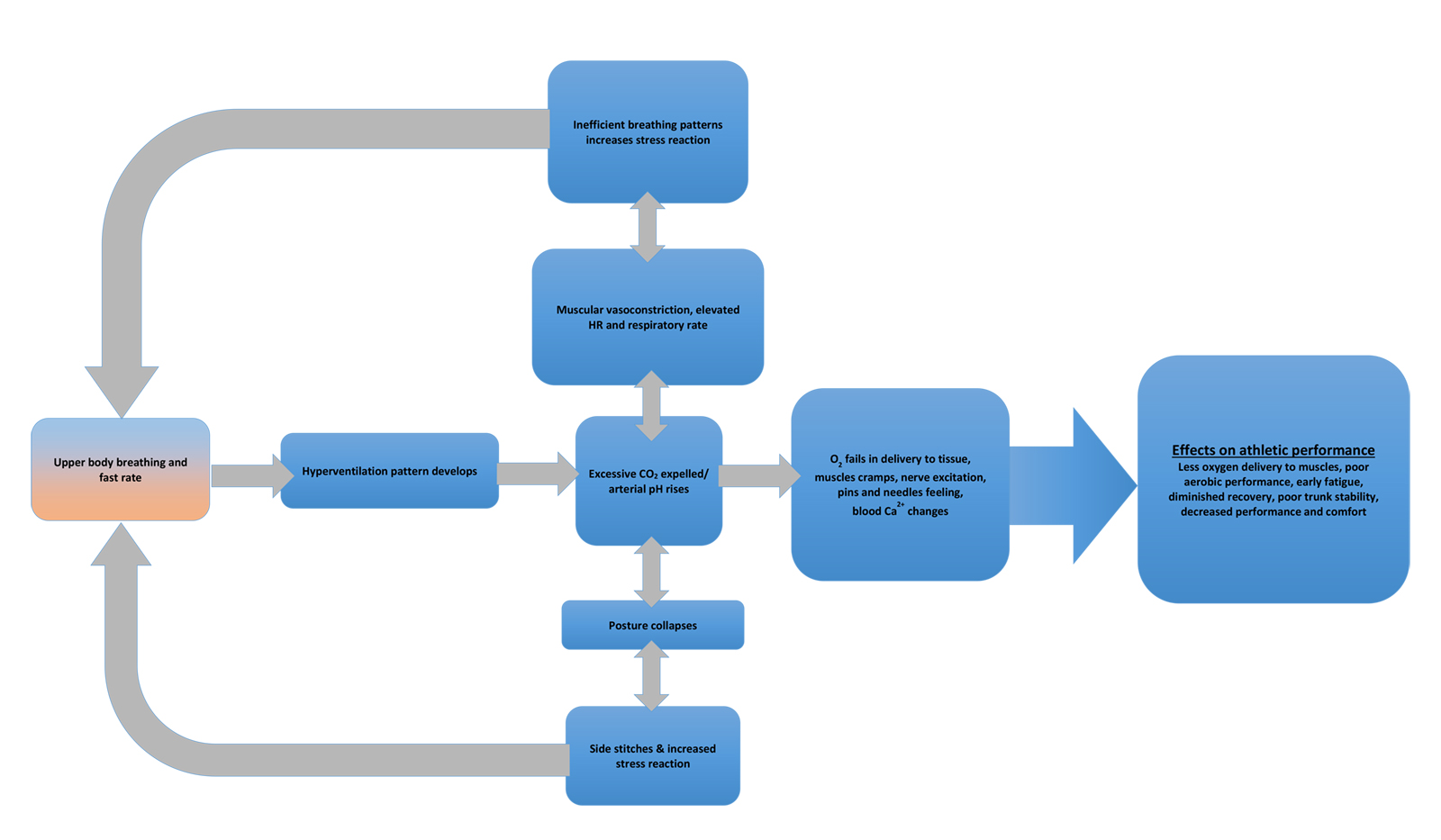
Dysfunctional breathing initiates a cycle in which the body’s nervous system is stimulated towards a fight or flight stress response (Sympathetic), with a cascade of ensuing symptoms. The above chart is a simplified version of one presented by Chaitow, and illustrates the major effects. Stress hormones are released by the adrenal glands, heart rate and contractility increases, posture begins to deteriorate, sweating is increased, and blood vessels constrict among other predictable symptoms. All of these increase anxiety and respiration rate, thus producing a feed forward loop in which the symptoms act to increase the breathing disorder.
Ultimately, the increased respiration rate leads to an excess of carbon dioxide emissions, and the body enters a state of hypocapnia (low blood CO2 concentration). The individual may begin to experience tingling in the extremities and exhaustion in addition to the symptoms outlined above. If allowed to go unresolved, respiratory alkalosis is attained (an increase in blood pH) that can be lethal to the body’s tissues. As a result, the body tries to regulate by releasing Calcium. This hypocalcaemia (low blood calcium concentration) involves muscle and nerve changes that can manifest as muscle spasms, lightheadedness, bronchospasms, neural irritability and even loss of consciousness in its most extreme manifestation.
Common symptoms of hyperventilation:
- Side stiches
- Dizziness/lightheadedness/fainting during or after exertion
- Frequent tenderness, and tightness in shoulders, neck, and chest
- Collagen injuries such as Achilles tendonopathy or plantar fasciitis
- History of low back pain related to exercise or certain postures
- Chest pain which may be related to breathing cycle
- Tingling in upper extremities or around mouth
- Cramping in calves, hands, or feet
- Headaches
An individual’s specific cluster of symptoms will likely differ, but running populations will often include several of the bullet points above. In his book, Chaitow suggested, “The symptoms of hyperventilation are diverse. None is absolutely diagnostic”.
How’s YOUR breathing serving you?
Here are some simple self-assessments to help you understand your breathing and body a little better.
What are you feeling?
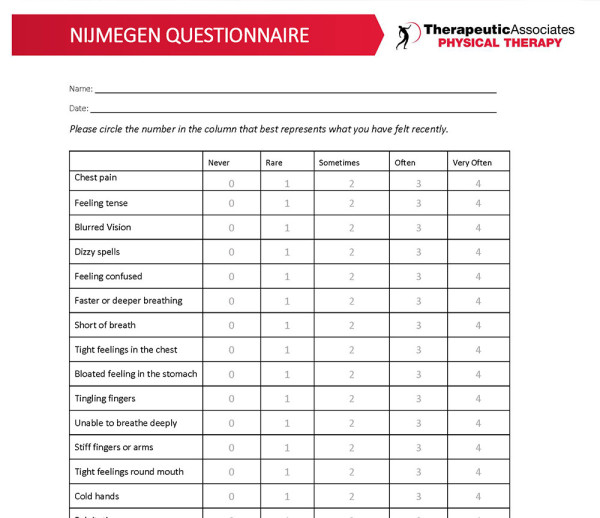
Nijmegan questionnaire (NQ):
The NQ is a very quick and simple screen for dysfunctional breathing. No tool by itself has the power to diagnose a breathing disorder but this one is a good start. Evidence supports this tool in helping to identify breathing dysfunction. (Dixhoorn, 2012)
Scores above 19 are considered indicative of potential breathing dysfunction that may benefit from breath related work (Dixhoorn, 2015). If you’re above 19 or just plain interested in hearing more, keep reading.
How are you positioned?
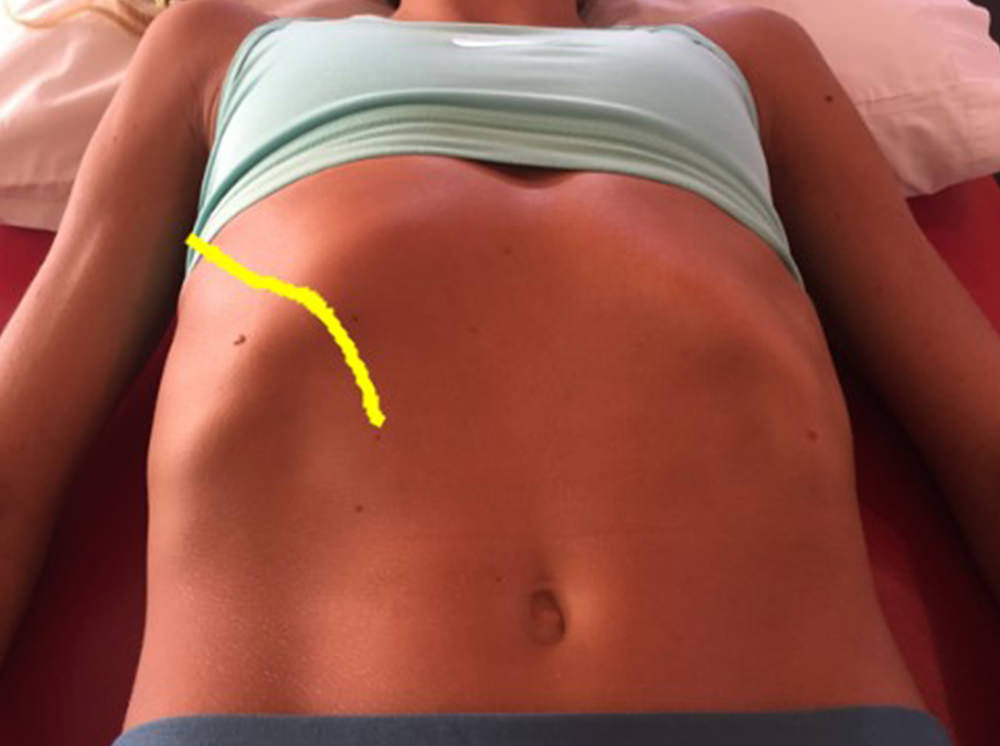
Rib Flare Test or the BradCliff® Ski Jump Test:
While lying on your back with knees bent and feet flat, feel the lower portion of the ribs just above the abdomen. The ribs should naturally flow into the abdominal musculature (soft tissue). If the bottom edge is easily palpable and appears like a ski jump going downwards off the ribs, this is potentially indicative of hyperinflation pattern (ribs “stuck” upwards). Rib Flaring is often more evident on the left due to our internal organ anatomy. If it’s minimal don’t panic. If it’s pronounced, you’re going to find some valuable information later in this article
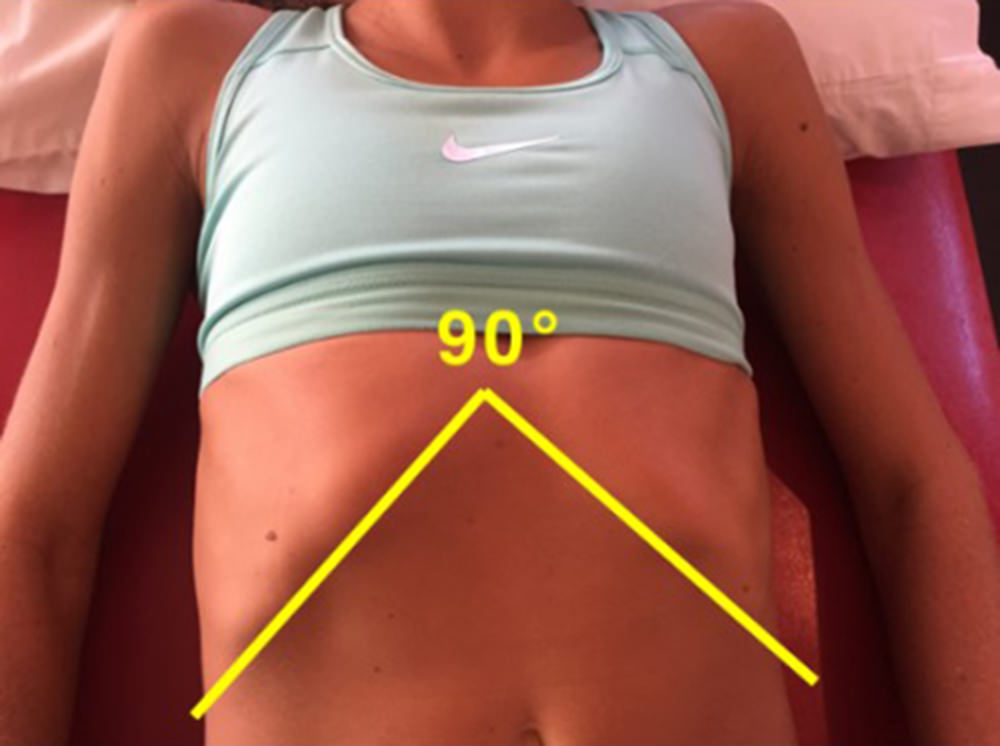
Infracostal Angle Test
This one is a little harder to do on your own but give it a try. Lying face up, feel the lower border of the lowest ribs, from the lowest part of the sternum out laterally. Appreciate the angle formed by the lower rib lines on each side. Most believe this angle should be around 90 degrees. If abdominal muscles are over active, the angle may be smaller and consequently narrowing that angle.
What's moving when you breathe?
HiLo Test:
While lying on your back with knees bent and feet flat, feel the lower portion of the ribs just above the abdomen. The ribs should naturally flow into the abdominal musculature (soft tissue). If the bottom edge is easily palpable and appears like a ski jump going downwards off the ribs, this is potentially indicative of hyperinflation pattern (ribs “stuck” upwards). Rib Flaring is often more evident on the left due to our internal organ anatomy. If it’s minimal don’t panic. If it’s pronounced, you’re going to find some valuable information later in this article
TAKE A DEEP BREATH! And let’s fix the problem
Important disclaimer: Let’s get the obvious business out of the way. If something feels significantly wrong, get it checked out by a professional. If you have unexplained chest pain, breathlessness, dizziness, or other alarming symptoms, consult a skilled medical practitioner before attempting to self-treat.
Next, we’ve created a multi-phase plan that will improve your breathing and performance. A large spectrum of severity exists for people suffering a Breathing Pattern Disorder. Some will complete all phases while others may find their answer in just the first 1-2 phases. Respiration is the single autonomic function we can exert the most conscious control over and through some simple interventions we may be able to ameliorate the condition.
Phase 1 Training: Cognitive Weeks 1-2
First, it is necessary to get your body’s respiratory strategy primed during a resting state before jumping straight to the intense demands of exercise. The initial phases of treatment involve training a new motor pattern. Just like swinging a tennis racket or playing guitar, at first this takes tremendous concentration, but with effort the practice becomes easier and ultimately automatic. Principles of motor learning show us that these acts generally take 4-6 weeks so practice with patience. An entrained breathing disorder may produce symptoms and be quite comfortable at the same time, while a new and healthier strategy may seem foreign at first and even stress the body into thinking it’s starving for air. Our first encouragement is to allow respiration to relax into a healthier pattern. Two interventions can be helpful in training this initial effect.
Quiet Nasal Diaphragmatic Breathing:
Some people misinterpret the idea of taking a “deep breath” as quickly gulping in as much air as possible, when in actuality it suggests to take an elongated diaphragmatic breath to facilitate a relaxing effect. Mouth breathing and dysfunction often present together and initiating intervention through simple nasal breathing can introduce a variety of beneficial effects. Amongst other differences, the nose provides twice the mouth’s passive resistance to breathing, causing us to naturally decreased respiration rate. It also improves O2 and CO2 circulation in the blood, improves lung volumes, and facilitates a relaxing response. All of the above effects act to shift the patient’s resting respiratory condition towards the healthy normal, through a simple intervention that can be practiced several times a day. This is especially effective when confronted with regular anxieties such as situational stress, stubbing your toe, the discomfort during a deep tissue massage or pre-race jitters. By conditioning a healthy response to these stresses, the carryover to athletic exertion will come more naturally.
90/90 Balloon Blow:
Flattening of the diaphragm and alterations in posture are inherent characteristics of breathing dysfunction, and correcting can lead to both immediate and long-term effects. Improved nervous system regulation, low back stabilization, and depth of breath can all resonate from this simple exercise of exhaling against resistance. Similar to nasal breathing, this encourages us to slow our rate by facilitating our neuromuscular programing to operate in a longer exhalation phase. And finally, it enables slight abdominal contraction to resist the balloon’s pressure while a breathing cycle continues, similar to the postural demands asked of the core while running. This intervention has been used to treat many more conditions, so giving it a quick attempt can be easy and possibly very effective.
Phase 2 Training: Integrative Weeks 2-4
Now that you’ve laid the foundation of learning a new breathing style, you’re ready to carry that in to something more functional, which will further help integrate your new skill in to your movement habits and in to your daily activities. We’ve found that the best way to start this is to integrate your new breathing patterns in to your stretching; instead of counting seconds, count your breaths. We suggest holding each stretch for 8-10 breath cycles, but we also realize there still exists conflicting theories of how long stretches should be held. Therefore, decide how long you’d like to hold each stretch and then time how many breath cycles that is for you. While in your stretch be attentive to your new diaphragmatic breathing habits and count your breath cycles. You might realize that not only does this start to tie your new breathing mechanics in to your functional activities, but also might allow you to relax more in to your stretching since the diaphragmatic style will trend you away from the sympathetic fight or flight response and more toward a relaxing state.
Phase 3 Training: Associative Weeks 4-6
The first phase focused on mastering a new motor program, the second phase starts to tie that in to some of your easy training while this third phase starts to implement that new breathing style into more complex movement skills. This becomes more challenging than you might think. It will be easy to revert back to your poor breathing habits as soon as you try to integrate them into complex movement tasks, so approach this phase with awareness and a realization that it might initially be a frustrating process.
By this point your diaphragmatic breathing will be more relaxed and exercise sessions can have a breathing mechanics check-in about every 5-10 minutes. This can be during an easy portion of the run, recovery jog during intervals, during your strength and conditioning program or during any other low intensity activity.
Here are a few exercises that might continue to help tie your new breathing patters in to your running mechanics.
Runner Balloon Blow:
Similar to the balloon blow exercise you’ve already done on your back; this just takes that skill in to your strong running posture.
Runner’s Touch:
Before a person can be expected to maintain posture explosively or over great distance, we must coordinate strength, balance, and movement slowly. This strength exercise is implemented with runner’s regularly to establish effective spinal stability, gluteal participation, and movement fluidity. Regardless of condition or presence of ailment, every competitive runner should be able to complete this fundamental exercise at any time.
Chops and Lifts:
This activity should look like lifting an object diagonally across your body or chopping down a tree. This activity coordinates spinal and upper extremity motion while in a split leg position, requiring extra postural demands from the diaphragm and abdomen.
Phase 4 Training: Automatic Weeks 6+
Now it is absolutely necessary to check in with breathing while exercising. Every 10 minutes, spend 1 minute focusing on inhaling deep into the lower abdomen and pelvis and exhaling for slightly longer. Acquiring a cadence can be helpful, such as inhalation of 2 seconds and exhalation over 3 seconds. This has the added benefit of being an odd numbered cycle, thus altering your muscle focus on to opposite legs each cycle for symmetry. Faster paces will likely necessitate faster cadences; so don’t feel you need to lock yourself to one cadence. There is a growing body of research exploring the coordinating of breath cycles to foot strike, but is beyond the intent of this article. All we ask in this phase is to start being more cognoscente during your runs, races and workouts about how you’re brining your healthier breath mechanics in to your training and racing. This can be a challenging process, but one that might make tremendous impact in your training and race potential.
Wrap Up
This document has been created to help raise awareness of all too common breathing pattern dysfunctions. Our hope is to help you find your best breathing. This topic has tremendous depth, with a variety of presentations and overwhelmingly diverse implications throughout the body. We’ve tried to simplify the highlights and pull out the low hanging fruit that we feel have the best potential to help. If this doesn’t feel like enough, find a local breathing expert to help take you further down this path. If you have any comments, success stories or questions feel free to reach out to us; we’d be happy to hear from you!
References
Aydogdu O, Sari Z, Aydin Ö, Yurdalan U. The effects of supervised and home-based breathing exercises on functional outcomes in patients with fibromyalgia syndrome. Eur Respir J. 2015;46(suppl 59):PA3536. doi:10.1183/13993003.congress-2015.pa3536.
Barker NJ, Jones M, O’Connell NE, Everard ML. Breathing exercises for dysfunctional breathing/hyperventilation syndrome in children. Cochrane database of Syst Rev. 2013;(12).
Boyle, KL, Olinick, J, Lewis, C. The Value of Blowing Up a Balloon. N Am J Sports Phys Ther. 2010;5(3):179–188.
Bradley H, Esformes J. Breathing Pattern Disorders and functional movement. The Int J Sports Phys Ther. 2014;9(1):28-39.
Chaitow L, Gilbert C, Bradley D. Recognizing And Treating Breathing Disorders. 2014
Daley MA, Bramble DM, Carrier DR. Impact Loading and Locomotor-Respiratory Coordination Significantly Influence Breathing Dynamics in Running Humans. PLoS ONE 2013;8(8).
Dixhoorn, JV, 2012. Nijmegan Questionnaire in the evaluation of medically unexplained symptoms, including hyperventilation complaints. Biological Psychology (in press)
Dixhoorn, JV, Folgering, H, 2015. The Nijmegan Questionnaire and dysfunctional breathing. ERJ Open Res (in press)
Gilbert, C. Better Chemistry through Breathing: the Story of Carbon Dioxide and how it can go wrong. Biofeedback. 2005:100–104.
Grammatopoulou, EP, Skordilis, EK, Stavrou, N, et al. The Effect of Physiotherapy-Based Breathing Retraining on Asthma Control. Journal of Asthma. 2011;48(6):593–601.
Han, J, Stegen, K, Simkens, K, et al. Unsteadiness of breathing in patients with hyperventilation syndrome and anxiety disorders. Eur Respir J. 1997;10(1):167–176.
Hodges PW, Butler JE, Mckenzie DK, Gandevia SC. Contraction of the human diaphragm during rapid postural adjustments. J Physiol 1997;505(2):539–548.
Hodges PW, Gandevia SC. Activation of the human diaphragm during a repetitive postural task. J Physiol 2000;522(1):165–175.
Hodges PW, Heijnen I, Gandevia SC. Postural activity of the diaphragm is reduced in humans when respiratory demand increases. J Physiol 2001;537(3):999–1008.
Jones M, Harvey A, Marston L, O’connell NE. Breathing exercises for dysfunctional breathing/hyperventilation syndrome in adults. Protocols Cochrane Database of Systematic Reviews 2013.
Key J. ‘The core’: Understanding it, and retraining its dysfunction. J Bodyw Mov Ther 2013;17(4):541–559.
Kolar P, Sulc J, Kyncl M, et al. Stabilizing function of the diaphragm: dynamic MRI and synchronized spirometric assessment. J Appl Physiol 2010;109(4):1064–1071.
Lee L-J, Chang AT, Coppieters MW, Hodges PW. Changes in sitting posture induce multiplanar changes in chest wall shape and motion with breathing. Respir Physiol Neurobiol 2010;170(3):236–245.
Park JW, Kweon M, Hong S. The influences of position and forced respiratory maneuvers on spinal stability muscles. J Phys Ther Sci 2015;27(2):491–493.
Rapee, RM. A case of panic disorder treated with breathing retraining. J Behav Ther Exp Psychiatry. 1985;16(1):63–65.
Smith, MD, Russell, A, Hodges, PW. Disorders of breathing and continence have a stronger association with back pain than obesity and physical activity. Aust J Physiother. 2006;52(1):11–16.