Kneecaps really aren’t a big deal. They sit there, minding their own business until they start to hurt a little, then a little more, and then … Yeah, it really starts to hurt, and they become a big deal.
Patellofemoral Pain Syndrome (pain around the kneecap) is one of the most common musculoskeletal problems in young athletes.1 Typical signs and symptoms include pain/soreness around the kneecap, pain using stairs, and pain with deep squatting or jumping.
In addition to young athletes, runners commonly experience Patellofemoral Pain Syndrome when increasing mileage and when resuming activities after periods of rest. It’s painful enough to finish out a race and can be miserable if you must battle through knee pain in the process.
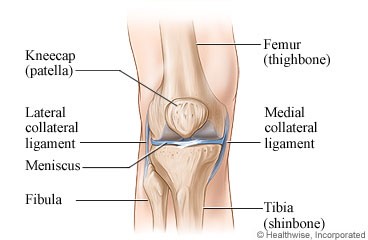
The kneecap sits in a small groove along your femur as pictured to the right. It typically gets irritated on the back side when not tracking properly within its groove or is under excessive compression.
Symptoms: How do You Diagnose Patellofemoral Pain Syndrome?
Diagnosis consists of recreating pain at the kneecap, then ruling out similar conditions. Symptoms your physical therapist will analyze during assessment and diagnosis include:
- Pain along the underside of the kneecap
- A decrease in pain with proper kneecap positioning via taping into an optimal position
- Pain with compression to the kneecap
- Pain with deep squatting
- Lack of tenderness to other knee structures
While there are other tests that can be implemented for diagnosis, through clinical experience, the above tests typically provide the most accurate answers.
Causes: Why Do You Get Patellofemoral Pain Syndrome?
It was once thought that when the inner quadriceps muscle (the muscle on the inside front of the thigh) was not working optimally, this was the main reason why the kneecap would become irritated. Stretching was the gold standard of treatment. However, patients weren’t getting better consistently.2
Other common treatments consisted of ice, rest, ultrasound, and electrical stimulation. Although beneficial in some cases, many patients were still failing to get better.
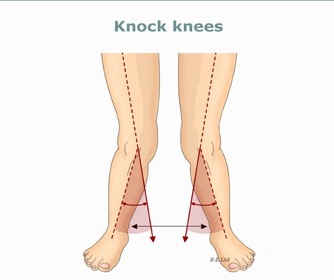
Recent research has shown that there are other biomechanical influences that likely lead to pain in the kneecap. It seems that the biomechanics of movement mainly cause the development of patellofemoral pain.3-5 A large knee valgus angle (“knock knees” as pictured to the right) causes irritation at the joint.
This knee position can be observed while standing or can happen during movement. As the femur moves into an inward position below the kneecap, the kneecap cannot maintain its proper position. So, this leads to irritation. Typically, we observe this in patients when they’re landing from a jump, during running, or when squatting.
Treatment: How Do You Fix Patellofemoral Pain Syndrome?
Initially, placing the kneecap in its proper position (taping it so that it better lines up with the femur) will help with irritation and typically has a drastic reduction in pain with normally painful activities.6 Ensuring the joint below the kneecap also has full hyper-extension will help properly seat the kneecap, which is typically accomplished through hands-on mobilizations and follow-up exercises.
After reducing the irritation and regaining full hyper-extension, it’s important to treat the joints above and below the knee including the ankle/foot, hip, and trunk. Improving the arch position of the foot, strengthening the side and back of the hip, and ensuring normal trunk position can all help in decreasing the ‘knock-kneed’ pattern and ensure the kneecap is aligned properly.7-11
Recent research suggests specific and isolated hip strengthening exercises provide excellent results.12 These exercises target your hip abductors (muscles that move your leg out to the side from the hip) and external rotators (muscles that rotate the leg in an outward direction). In one particular study, patients reduced their average pain from 8/10 to about 1/10 after simply performing high repetitions of these exercises 3 times per week for 8 weeks.
References:
1. DeHaven KE, Lintner DM. Athletic injuries: comparison by age, sport, and gender. Am J Sport Med.1986;14:218–224. [PubMed]
2. Dolak KL, Silkman C, Medina McKeon J, Hosey RG, Lattermann C, Uhl TL. Hip strengthening prior to functional exercises reduces pain sooner than quadriceps strengthening in females with patellofemoral pain syndrome: a randomized clinical trial. J Orthop Sports Phys Ther. 2011; 41: 560– 570.[Medline]
3. Powers CM. The influence of abnormal hip mechanics on knee injury: a biomechanical perspective. J Orthop Sports Phys Ther. 2010; 40: 42– 51. [Medline]
4. Powers CM. The influence of altered lower-extremity kinematics on patellofemoral joint dysfunction: a theoretical perspective. J Orthop Sports Phys Ther. 2003; 33: 639– 646. [Medline]
5. Souza RB, Draper CE, Fredericson M, Powers CM. Femur rotation and patellofemoral joint kinematics: a weight-bearing magnetic resonance imaging analysis. J Orthop Sports Phys Ther. 2010; 40: 277–285. [Medline]
6. Whittingham, M, Palmer, S, Macmillan, F. Effects of Taping on Pain and Function in Patellofemoral Pain Syndrome: A Randomized Controlled Trial. Journal of Orthopaedic & Sports Physical Therapy, 2004 Volume:34 Issue:9 Pages:504–510
7. Eng JJ, Pierrynowski MR. Evaluation of soft foot orthotics in the treatment of patellofemoral pain syndrome. Phys Ther. 1993; 73: 62– 68; discussion 68–70. [Medline]
8. 40: 736– 742. http://dx.doi.org/10.2519/jospt.2010.3246 [Abstract] [Medline]
9. Earl JE, Hoch AZ. A proximal strengthening program improves pain, function, and biomechanics in women with patellofemoral pain syndrome. Am J Sports Med. 2011; 39: 154– 163. [Medline]
10. Mascal CL, Landel R, Powers C. Management of patellofemoral pain targeting hip, pelvis, and trunk muscle function: 2 case reports. J Orthop Sports Phys Ther. 2003; 33: 647– 660. [Medline]
11. Fukuda TY, Rossetto FM, Magalhaes E, Bryk FF, Lucareli PR, de Almeida Aparecida Carvalho N.Short-term effects of hip abductors and lateral rotators strengthening in females with patellofemoral pain syndrome: a randomized controlled clinical trial. J Orthop Sports Phys Ther. 2010;
12. Khayambashi K, Mohammadkhani MS, Ghaznavi, K, Lyle M, Powers C. The Effects of Isolated Hip Abductor and External Rotator Muscle Strengthening on Pain, Health Status, and Hip Strength in Females With Patellofemoral Pain: A Randomized Controlled Trial. Journal of Orthopaedic & Sports Physical Therapy, 2012 Volume:42 Issue:1 Pages:22–29 DOI:10.2519/jospt.2012.3704
We’re here to help you reach your goals.
If you’re experiencing pain at the front of the knee, or in and around the kneecap, you are not alone. Patellofemoral Pain Syndrome is a common type of knee pain, particularly in young athletes and active adults of all ages who increase their activity level abruptly, especially if the activity involves repetitive knee motion such as running. Physical therapy can help.