You walk into a local shoe store to find something for your running or walking routine. You have had foot pain before, and you do not want that to happen again. A friend told you about anti-pronation shoes, which helped with their foot pain. Then you stop and think to yourself, what is pronation? Is it bad? Could that be the culprit of my foot pain? What can I do to stop it? Keep reading and you will soon see that pronation may not be what you think.
Introduction
In this blog, we will describe pronation and its effect on our foot health. Good foot health is important for living an active, healthy lifestyle. Having healthy feet will encourage you to keep walking, swimming, biking, running, participating in sports, etc., which will in turn keep you healthy and satisfied for a long time to come. We will also discuss “pes planus,” or flat feet, which is having pronated feet while you are standing in a static position. This is when the foot’s arch is closer to or touching the ground. It is estimated that 20 to 37 percent of the population has pes planus. Pronation and pes planus have been implicated as causes of foot and ankle pain for decades and as a result, people are spending hundreds of dollars on ‘anti-pronation’ shoes, orthoses (shoe inserts) and all kinds of other equipment to prevent or manage pain. Is that necessary?
What is overpronation?
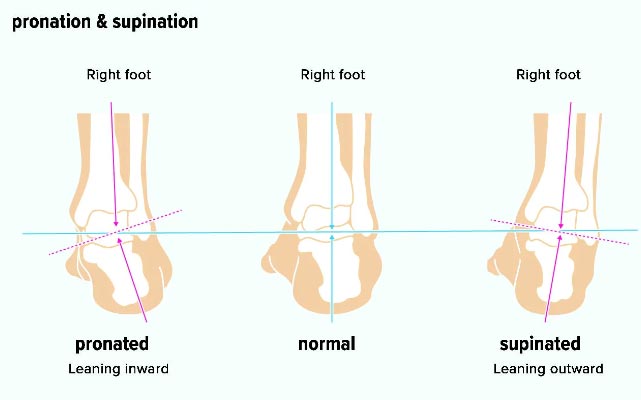
Pronation refers to a natural movement of your foot. It is the term that describes the time just after your heel touches the ground and while you are distributing your body weight onto your foot. As you walk or run, your heel hits the ground, followed by the rest of your foot as you move forward. There is a small amount of mid-foot movement toward the inside or inward rolling of the foot, and your arch will move closer to the ground. Pronation acts like a spring and allows for shock absorption and adjustment to terrain, and it helps maintain equilibrium.
Overpronation is when the mid-foot rolls too much, causing the arch of the foot to flatten and sometimes touch the ground. This is analogous to the spring being overly stretched, which causes difficulty and delay in returning to its resting position.
There are many possible causes of overpronation. For some, it is as simple as weakness in specific muscles in the foot that allow the arch to flatten. It may also be a matter of habit, not weakness. People may get used to standing with this foot posture despite relatively normal foot strength. Footwear can also alter foot muscle use and therefore foot postural strength.
For example, a review of several studies demonstrated that rocker bottom shoes can inhibit use and weaken muscles in the front portion of the lower leg and activate the calf muscles instead. Also, this review pointed out a few studies that demonstrated that foot orthoses can limit muscle activity in the inner part of the leg and activate muscles opposite, on the outer leg. This may lead to an imbalance of muscle strength in the lower leg, leading to altered foot posturing.
Overpronation can be also caused by genetics, which can impact the shape of the bones in your foot and your foot itself. There are also rare genetic conditions that can cause overpronation because of an increase in the flexibility in the tendons and ligaments that hold the foot bones together – examples include Ehlers-Danlos Syndrome, Down Syndrome and Marfan’s Syndrome. It can also be caused by injury or trauma to tendons in the foot, such as the posterior tibialis tendon, as well as by injury to many of the ligaments that support the foot or ankle.
Effects of overpronation on foot health
The current evidence from research is unclear as to how much overpronation really contributes to injury. Overpronation has been linked to the most common running-related injuries such as shin splints, Achilles tendinopathy, plantar fasciitis, patellar tendinopathy and anterior knee pain. However, the debate among researchers is trying to determine if overpronation is the cause of these injuries or just a correlation. Many people have what would be defined as overpronation, but they have no pain at all.
A study by Garbalosa et al. surveyed 234 people with painless, healthy feet, and found that less than 5 percent had the “ideal” neutral foot posture.
It is possible that overpronation is just an innocent bystander. Ian Griffths, an accomplished podiatrist and researcher, has said, “it has often been assumed that foot posture may be one of the contributing factors in a presenting lower limb injury (which, of course, it may well be for some). The subtle differences between causation and correlation should always be kept in mind. Just because a foot/lower limb that hurts is pronated, does not mean that it hurts because it is pronated. This is why a thorough history of the mechanism of the presenting injury and all other potential contributing factors are just as important as foot posture and should be concurrently investigated.”
What are these other contributing factors? Another researcher, Marc A. Raj, summed up two research articles and stated, “The main factors that contribute to an acquired flat foot deformity are excessive tension in the (calf muscles), obesity, posterior tibial tendon dysfunction, or ligamentous laxity in the … plantar fascia, or other supporting plantar ligaments. It may also result from a tight Achilles tendon or calf muscle.”

Interestingly, some research has proposed that supposed overpronation can be beneficial. Wen et al. looked at the foot alignment of marathon runners and found that participants with greater heel valgus (an important part of pronation) were less likely to sustain an over-use injury.
Diagnosing overpronation and other foot structures
Because each foot is distinct in its structure and in the way it moves, and because so many tissues and structures contribute to foot health, everyone with foot/ankle pain should be evaluated on a case-by-case basis by an expert in anatomy, physiology and biomechanics. This expert should also be well-versed in the latest evidence-based treatments for your condition. Physical therapists are uniquely qualified to assess muscle strength, joint mobility, biomechanics, gait pattern and running strategy. They can help in myriad ways to get you back to walking and running comfortably again.
During the evaluation, a physical therapist will want to hear your whole story and will ask questions to obtain a thorough background about the timing of symptoms, severity of past and current symptoms, history of trauma, family history, surgical history and medical history. Next, the therapist will perform a physical exam and assess your joint mobility, your movement patterns (such as what your foot does when you squat, or balance, or hop), your ligament stability, and your muscle strength, range of motion and walking/running patterning.
Note that physical therapists are part of the healthcare community in which they live and will have connections to a multi-disciplinary team including podiatrists, orthopedic specialists, orthotic specialists, radiologists, etc., to help you receive the most complete care and treatment.
Treatment for overpronation
Pes planus or overpronating can be a small piece of a large puzzle. Research shows that pes planus and overpronation can be contributing factors to foot, ankle, knee and even hip pain. Once a physical therapist has concluded a thorough examination, they will determine if you have overpronation, and to what extent it may be contributing to your pain. They will also determine if there are other contributing factors and will create a customized treatment plan tailored to your individual needs.
Usually, physical therapists will use this general framework to optimize the healing process:
- Temporarily offload to decrease stress/strain to the specific painful tissue (muscle, tendon, ligament, etc.) and allow time for healing
- Gradually re-introduce load (weight, force) to strengthen the muscles and tendons as tolerated by the patient
- Optimize movement patterns to minimize the risk of re-injury
Treatment may include using hands-on techniques to mobilize joints that have become stiff or to relax tight or painful muscles and tendons. Specific exercises may be given to stretch the stiff joints and tight muscles and to strengthen those muscles that may have become weak or have not been performing optimally.
A physical therapist may also recommend using foot orthoses to decrease the specific load on a tissue for a time to allow for optimal healing. It is important, however, to gradually increase the load again to promote muscle and tendon healing and re-strengthening. This may mean that the orthoses may only be used for a time and then weaned until the foot has become strong enough to function properly. Talk with a physical therapist to determine what the best course will be for you.

Preventing overpronation
An ounce of prevention is better than a pound of cure. Here is some advice to prevent foot and ankle pain in the first place.
- During your exercise and training process, it is important to gradually and incrementally increase load, speed, or distance such that your body can recover and build itself up to meet the new demands. A good rule of thumb is to stop and rest if your pain level reaches 4-5 out of 10 during an activity. Also, directly after an activity, soreness/pain should not last more than 1-2 hours. If it does, decrease the intensity of that activity. Soreness that occurs 12-48 hours after an activity is normal after an increase in training but should not last more than a day or two.
- Foot orthoses. Unless you are already wearing foot orthoses consistently, it is not suggested that you do so to prevent injury. They can be a great tool to decrease pain as described above; however, like a crutch, they can limit the movement of your foot and therefore the strength of your fe Because the muscles are not being used, they can become weaker over time and potentially cause problems in the future.
- Changing shoes. It is recommended to replace running shoes after 300 to 500 miles of running or activity. You can also look for signs of wear such as the midsole feels soft and collapses easily under pressure, longitudinal creases appear in the midsole, the heel becomes mobile and unsupportive, your toes wear through the toe-box or the shoe upper tears. A feeling of increased muscle soreness after running in a pair of well-worn shoes should prompt further investigation of their structural integrity.
Conclusion
Let’s recap!
- Pronation is a natural movement that should not be feared. Some have more than others and research has not conclusively shown that overpronation causes more injuries compared to other foot postures.
- Foot and ankle pain is often complex and multifactorial and should be treated by an expert.
- Physical therapists —k.a. the movement experts — are uniquely equipped with the knowledge to expertly assess the foot posture, anatomy and biomechanics that lead to your specific walking and running gait patterns. They can create and execute customized treatment plans to optimize your movement.
So, if you are experiencing foot or ankle pain, do not hesitate to reach out to your local physical therapist and get on the road to recovery and return to doing what you love.

Feet hurt? See a physical therapist today!
As physical therapists, we know the importance of movement for overall health and well-being. From injury recovery to achieving optimal performance, our passion is to help every patient reach their goals and live an active, pain-free life. Get started with PT today!
References:
- (https://www.jospt.org/doi/10.2519/jospt.2021.9710)
- (Munro BJ, Steele JR. Foot-care awareness. A survey of persons aged 65 years and older. J Am Podiatr Med Assoc. 1998 May;88(5):242-8.)
- Garbalosa JC, McClure MH, Catlin PA, et al. The frontal plane relationship of the forefoot to the rearfoot in an asymptomatic population. Journal of Orthopaedic & sports Physical Therapy 1994;20:200– 206)
- (Wen Dy, Puffer JC, Schmalzried TP, et al. Injuries in runners: a prospective study of alignment. clinical Journal of sport medicine 1998;8:187–194)
- Marc A. Raj https://www.ncbi.nlm.nih.gov/books/NBK430802/#:~:text=It%20is%20estimated%20that%20about,some%20degree%20of%20pes%20planus.
- https://www.asics.com/gb/en-gb/asics-advice/changing-your-running-shoes-knowing-when-is-the-right-time.html
